T cells in peripheral immunity
-
Project Leader

Professor Francis (Frank) Carbone+61 3 8344 9923
Project Details
T cells are key immune cells involved in protection against a broad range of microbes. T cells exist as distinct subsets that have specialised functions and roles during immune responses. Parts of our project aim at understanding how these diverse functions of T cells are regulated within infected tissues during the early stages of microbial invasion. Furthermore, we are interested in the generation and regulation of so-called memory T cells that emerge following the extensive contraction of the pathogen-specific T cell pool once infection has resolved (Figure 1). Memory T cells are key to immunity against re-infection and continuously patrol diverse organs for invading pathogens. We are particularly interested in this patrolling or immuno-surveillance function of memory T cells and are trying to understand how different factors can "imprint" organ-tropic migration in memory T cells.
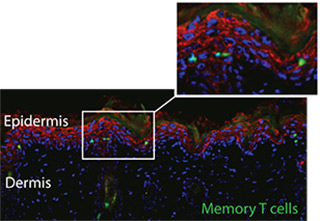
Figure 1: Virus-specific memory T cells (shown in green) persist in the epidermal layer of the skin (indicated by red keratin staining). Skin was analysed two weeks after skin infection with herpes simplex virus-1 (HSV-1).
Separately, there is recent evidence that certain peripheral tissues can support the generation of a distinct subset of killer memory T cells called tissue-resident memory T cells (TRM)(Figure 2). These cells differ from their recirculating counterparts found in the blood and permanently persist in tissues such as skin and mucosa. Given that these surface tissues are common portals of entry for pathogens, TRM cells are strategically well positioned to rapidly control re-infection. Parts of our project aim at understanding the generation and persistence of TRM in peripheral organs and at evaluating these cells as potential targets for future T cell vaccines. Our research program is funded by the NHMRC project grants #628423 "Effective T cell memory in peripheral organs" (Thomas Gebhardt) and #1003717 "The role of helper T cells in immunity to HSV-1" (Andrew Brooks and Thomas Gebhardt).
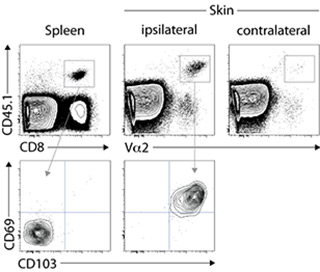
Figure 2: Virus-specific memory T cells persist in previously infected skin and display a unique phenotype. Analysis of memory T cells in spleen and previously infected (ipsilateral) or control (contralateral) skin (>1 year after HSV-1 infection). Rectangles indicate virus-specific memory cells as CD8+CD45.1+ or Va2+CD45.1+ events (upper panel). Lower panel shows the expression of CD103 and CD69 by circulating (spleen) and tissue-resident (skin) memory T cells.
Researchers
Thomas Gebhardt, Laura Mackay, Angus Stock, Bethany McLeod, Nicholas Collins, Sanda Stankovic
Research Group
Faculty Research Themes
School Research Themes
Molecular Mechanisms of Disease
Key Contact
For further information about this research, please contact the research group leader.
Department / Centre
MDHS Research library
Explore by researcher, school, project or topic.