University of Melbourne plays pivotal role in tackling snakebite worldwide
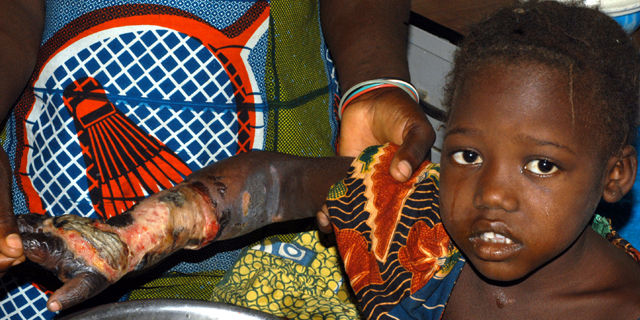
This child in Kaltungo, Nigeria, has been bitten by a West African carpet viper (Echis ocellatus) and is suffering from extensive tissue damage (necrosis). Photograph by David Warrell.
Improving treatment and reducing the death and injury toll from snakebites globally took a major step forward when the World Health Organization added snakebite to the highest priority list of Neglected Tropical Diseases (NTDs) this month.
The University of Melbourne has played a pivotal role in the move and one of its leading venom experts, Dr David Williams, has called for a concerted effort to minimise the massive health and economic impact that venomous snakes have world-wide.
“WHO’s landmark decision recognises the devastating impact of snakebite in some of the world’s poorest communities, and sends a strong message about the urgent need for the global community to develop effective controls that would save tens of thousands of lives each year,” he says.
“Venomous snakes bite five million people worldwide every year, claiming the lives of at least 125,000 and leaving more than 400,000 permanently disabled. But a global push for change is gaining momentum, and our Australian-based Global Snakebite Initiative has taken the lead.”
Dr Williams, who heads the Australian Venom Research Unit (AVRU) in the University of Melbourne’s Department of Pharmacology and Therapeutics, says the listing of snakebite as a ‘Category A Neglected Tropical Disease’ recognises the enormous toll it takes on some of the world’s poorest and most marginalised people.
As CEO of The Global Snakebite Initiative (GSI), Dr Williams leads AVRU’s snakebite project in Papua New Guinea, where a new antivenom to treat taipan bites developed in with PNG, Costa Rican, Spanish and UK partners has just finished clinical trials and is expected to save up to 1000 lives each year.
With AVRU colleague Diana Barr, Dr Williams worked with GSI members, secretariat partner Health Action International, a coalition of UN Member Nations led by the Government of Costa Rica, and the WHO for 18 months to push for the new classification.
“For decades the problem has been ignored by governments, aid donors and the pharmaceutical industry, leading to the current state of crisis in which many countries simply do not have access to safe, effective or affordable treatment,” Dr Williams says.
“The decision by WHO to recognise snakebite envenoming as an NTD, gives us the opportunity to finally change the future of snakebite outcomes for millions of people right around the world, and AVRU and GSI are committed to working with WHO to ensure the success of this effort.”
But Dr Williams says it is crucial that the rest of the world also gets behind WHO’s decision and provides it with the resources it needs to develop and implement an effective global snakebite control program. Future steps should include:
- improving the treatment of victims before, during and after hospital admission
- increasing the capacity of countries to ensure that antivenoms they use are safe, effective and appropriate to local snake species
- improving the supply, availability and regulatory oversight of appropriate antivenoms
- stimulating and supporting research into better diagnostic and therapeutic approaches
- helping manufacturers develop better antivenoms and ancillary treatments
- amplifying strategies to promote and encourage prevention and correct health-seeking behaviour at community level
- making snakebite a notifiable disease to improve the reporting of case numbers
- engaging with experts who can help people through physical, psychological and economic rehabilitation after snakebite.