White tailed Spiders

White-tailed spider (Lamponidae Lampona cylindrata; Photo by David McClenaghan, CSIRO)
White tailed spiders are readily identifiable by their cylindrical body shape and the presence of a white or grey spot on the end on their abdomen. They are active hunters, preying upon other types of spiders, and may be found roaming inside houses, especially in warmer weather.
White Tailed Spiders

(Photo A. Young, AVRU)
About
White tailed spiders are readily identifiable by their cylindrical body shape and the presence of a white or grey spot on the end on their abdomen. They are active hunters, preying upon other types of spiders, and may be found roaming inside houses, especially in warmer weather. White tailed spiders are readily identified by a distinctive white spot on the abdomen, present in both males and females. They are often found in bedding, or in clothing that has been left on the floor, and are mainly active at night, when they hunt for prey of spiders and insects. It is unknown whether the male and female are equally associated with skin necrosis. In most spider bite cases in which Lampona sp. have been positively identified, only a mild localised reaction or blister ensues. There is, however, a small number of cases of significant tissue loss after a witnessed bite by these spiders.
Distribution
White tailed spiders are found in most areas of Australia, and are common in urban dwellings
Venom
White tailed spiders have been implicated in some cases of Necrotising Arachnidism (skin breakdown or ulceration following spider bites). The incidence of ulceration or necrosis following white tailed spider bite is not known. The majority of cases appear not to develop ongoing ulceration, although blisters and redness are common.
About white tailed spider bite
Most cases of witnessed white tailed spider bites do not develop ongoing ulceration, although blisters and redness are common.
- A small number of witnessed white tailed spider bite cases have been associated with skin ulceration or necrosis (breakdown of the skin).
- The incidence (number of cases) of ulceration or necrosis following white tailed spider bite is not known.
- The majority of alleged cases of necrotising arachnidism in Australia are based on circumstantial evidence at best.
- There is currently no test available, clinically or experimentally, that can confirm or exclude the diagnosis of white tailed spider bite (or any other spider bite).
- There is currently no antivenom or other specific treatment for white tailed spider bite.
- No treatment has been shown in clinical or experimental trials to be of particular benefit in the treatment of ulcers ascribed to white tailed spider bites.
- Hyperbaric Oxygen Therapy has been used to treat ulcers of various origins, including suspected spider bite, with some success. There are case reports of its success in the healing of some ulcers thought to be due to spider bite, but no controlled trials have been conducted.
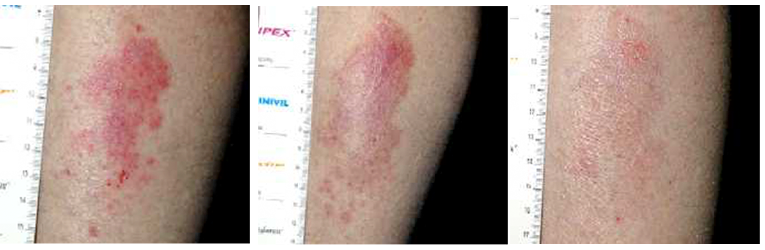
Photos: K. Hoyle
Do white-tailed spiders cause necrotic ulcers?
There is little evidence that bites from the white-tailed spider result in severe or necrotic ulceration. In a study of 130 patients with confirmed white-tailed spider bites, no cases of necrotic ulcers were observed (Isbister & Gray, 2003).
The notion that necrotic ulcers could be caused by bites of white-tailed spiders has been in the zeitgeist for decades. The belief stands that either the venom itself or bacteria in the venom of the spider result in a syndrome of blistering and ulceration or necrosis surrounding the bite site. While bacterial infections can certainly lead to necrotic injuries, no definitive link has been made between white-tailed spider bites and this condition.
To quote clinical toxinologist Prof Julian White (1999), "the white-tailed spider is often suspected but never confirmed to be the culprit. In most cases, a spider is found in the house after the bite and an unsubstantiated link is made.'